Diabetic retinopathy is a complication of diabetes that mainly affects the eyes and it is the leading cause of blindness especially among diabetic (both type 1 and 2) adults aged between 20 and 74 years. It occurs when elevated blood sugar levels damage the tiny light sensitive blood vessels and tissue inside the retina (at the back of the eye).
Stages of diabetic retinopathy
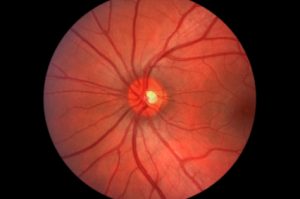 1. Mild non-proliferative retinopathy: This is the earliest stage that occurs when diabetes affects the circulatory system of the retina thus weakening the walls of retinal capillaries forming microaneurysms. Microaneurysms are small outpunches of the small blood vessels which can leak blood and fluid leading to edema and swelling in the retina which result in small dot-like hemorrhages.
1. Mild non-proliferative retinopathy: This is the earliest stage that occurs when diabetes affects the circulatory system of the retina thus weakening the walls of retinal capillaries forming microaneurysms. Microaneurysms are small outpunches of the small blood vessels which can leak blood and fluid leading to edema and swelling in the retina which result in small dot-like hemorrhages.
2. Moderate non-proliferative retinopathy: As the disease worsens or progresses the nourishing small blood vessels of the retina are blocked.
3. Severe non-proliferative retinopathy: As many more tiny blood vessels in the retina are blocked, several areas of the retina are deprived off blood and oxygen supply. In an attempt to maintain adequate blood supply, sends signals to the body to stimulate the growth of new fragile blood vessels in order to bring in nourishment.
4. Proliferative retinopathy: Once neovascularization (formation of new blood vessels in the retina) occurs the condition becomes worse. Proliferative retinopathy is mainly characterized by the growth of fragile abnormal tiny blood vessels both on the retinal surface and also on the vitreous gel inside the eye. If left untreated, these fragile and delicate blood vessels leak blood leading to severe vision loss or even blindness resulting from retinal detachment.
Signs and Symptoms of Diabetic Retinopathy
Patients are normally asymptomatic in the early phases of diabetic retinopathy. However, in the more advanced stages, complications may start developing and the patient may experience several symptoms including blurred vision, distortion, floaters, and acute progressive loss of vision. There are also other signs and symptoms of diabetic retinopathy which include;
- Microaneurysms: This is the earliest clinical symptom of diabetic retinopathy. They occur secondary to outpunch of capillary walls due to pericyte loss. They primarily appear as small red dots mainly in the superficial retinal layers.
- Dot and blot hemorrhages: If they are very small, they appear similar to microaneurysms. They occur as a result of rupturing of the microaneurysms in the deep layers of the retina such as the outer pexiform and the inner nuclear layers.
- Flame-shaped hemorrhages: These are splinter hemorrhages that mainly occur in the superficial nerve fiber layer.
- Hard exudates and retinal edema: These are caused by breakdown of the retina-blood barrier. This allows leakage of allowing leakage of lipids, serum proteins, and protein from the tiny blood vessels.
- Macular edema causes visual impairment.
- Complexity reading due to blurred or distorted vision.
- Pain in the eyes.
- Distorted central vision.
- Abnormal patterns or floaters in the field of vision.
Who is at risk of Diabetic Retinopathy?
Diabetics (both type 1 and type 2) are at risk of developing this and other eye diseases which can result in severe loss of vision and/or blindness. This can occur much earlier and is likely to be more severe is a person’s diabetes is poorly managed or left untreated. Additionally, pregnant women who are diabetic should guard their vision by having a comprehensive dilated eye examination.
Treatment of Diabetic Retinopathy
· Glucose control: Intensive glucose control especially in patients with IDDM (insulin dependent diabetes mellitus) decreases the progression and incidence of diabetic retinopathy.
· Laser photocoagulation: This entails the use of a high focused beam of light (energy) to stimulate a coagulative response.
· Pan-retinal photocoagulation: This procedure involves the application small laser burns over the retina in order to spark the central muscular area. This can eliminates the blood vessels completely and stop the leaking.
· Vitrectomy: This procedure is very effective in case of tractional retinal detachment, long standing vitreous hemorrhage, and combined rhegmatogenous and tractional retinal detachment. Treatment of diabetic retinopathy is often very successful especially in preventing, delaying or reducing loss of vision. However, all these procedures do not eliminate the disease entirely.
Prevention
Diabetic retinopathy can be prevented or slowed down by keeping all systemic parameters under control. Such systemic parameters include kidney function, blood sugar levels, lipid profile (triglycerides and cholesterol), hemoglobin levels, and blood pressure. Meditation practice is very effective in reducing and preventing stress. This helps prevent a rise in blood sugars. Moreover, mindful and responsible food choices supports healthy blood sugar level. Yoga and exercise are essential in the management of the blood sugar levels mainly because it helps move glucose into the muscle. On the other hand, yoga postures can be modified to accommodate diabetic people.
For more information, follow our suggested link.

